Frequently Asked Questions
- What is Gingivitis ?
- How do I know if I have Gingivitis ?
- How can I prevent Gingivitis ?
- What is Periodontitis ?
- How can I prevent Periodontitis ?
- Should I replace my silver fillings ?
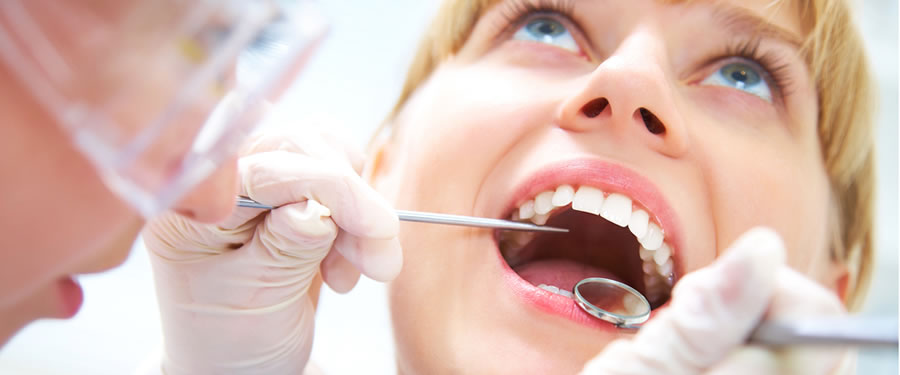
What is Gingivitis ?
Gingivitis - an inflammation of the gums - is the initial stage of gum disease and the easiest to treat. The direct cause of gingivitis is plaque; the soft, sticky, colorless film of bacteria that forms constantly on the teeth and gums. If the plaque is not removed by daily brushing and flossing, it produces toxins (poisons) that can irritate the gum tissue, causing gingivitis.
At this early stage in gum disease, damage can be reversed, since the bone and connective tissue that hold the teeth in place are not yet affected. Left untreated however; gingivitis can become periodontitis and cause permanent damage to your teeth.
Back to Top
How do I know if I have Gingivitis ?
Classic signs and symptoms of gingivitis include red, swollen and tender gums that may bleed when you brush. Another sign of gum disease is gums that have receded or pulled away from your teeth, giving your teeth an elongated appearance. Gum disease can cause pockets to form between the teeth and gums, where plaque and food debris collect. Some people may experience recurring bad breath or a bad taste in their mouth, even if the disease is not advanced.
Back to Top
How can I prevent Gingivitis ?
Good oral hygiene is essential. Professional cleanings are also extremely important because once plaque has hardened and built-up, or become tartar, only a dentist or dental hygienist can remove it.
You can help stop gingivitis before it develops by:
- Proper brushing and flossing to remove plaque and debris and control tartar buildup.
- Eating right to ensure proper nutrition for your jawbone and teeth.
- Avoiding cigarettes and other forms of tobacco.
- Scheduling regular checkups with your dentist.
Back to Top
What is Periodontitis ?
Periodontitis is a set of inflammatory diseases affecting the [periodontium], tissues that surround and support the teeth. Periodontitis involves progressive loss of the alveolar bone around the teeth and if left untreated, can lead to the loosening and subsequent loss of teeth. Periodontitis is caused by micro-organisms that adhere to and grow on the tooth's surface area, along with an overly aggressive immune response against these micro-organisms. A diagnosis of periodontitis is established by inspecting the soft gum tissues around the teeth with a probe and by evaluating the patients x-ray's of the gum and teeth to determine the amount of bone loss around the teeth.
Back to Top
How can I prevent Periodontitis ... ?
Daily oral hygiene measures to prevent periodontal disease include:
- Brushing properly on a regular basis (at least twice daily), with the patient attempting to direct the toothbrush bristles underneath the gum line, to help disrupt the bacterial-mycotic growth and formation of sub gingival plaque.
- Flossing daily and using interdental brushes (if there is a sufficiently large space between teeth), as well as cleaning behind the last tooth, the third molar, in each quarter.
- Using and antiseptic mouthwash in combination with careful oral hygiene may cure gingivitis, although they cannot reverse any attachment loss due to periodontitis.
- Regular dental checkups and professional teeth cleaning as required. Dental checkups serve to monitor the person's oral hygiene methods and levels of attachment around the teeth, identify any early signs of periodontitis and monitor response to treatment.
Typically dental hygienists (or dentists) use special instruments to clean (debride) teeth below the gum line and disrupt any plaque growing below the gum line. This is a standard treatment to prevent any further progress of established periodontitis. Studies show that after such a professional cleaning (periodontal debridement), microbe plaque tend to grow back to pre-cleaning levels after about 3 to 4 months. However, it is advocated that the interval between dental checkups should be determined specifically for each patient between every 3 to 12 months.
Note: Periodontal disease and tooth loss are associated with an increased risk of oral cancer.
Back to Top
Should I replace my silver fillings ?
Silver fillings are like other products that have a useful life expectancy. As in any other product that has a "use by date", all dental fillings have a "use by date". A proper examination, utilizing an intra-oral camera can help determine whether or not a filling has surpassed it's "use by date". Old silver fillings expand through corrosion with age, usually after ten years, causing the tooth enamel to crack. A mush better restoration in today's dentistry is a bonded, ceramic restoration which is tooth colored, doesn't expand with time and strengthens the tooth rather than weakening it.